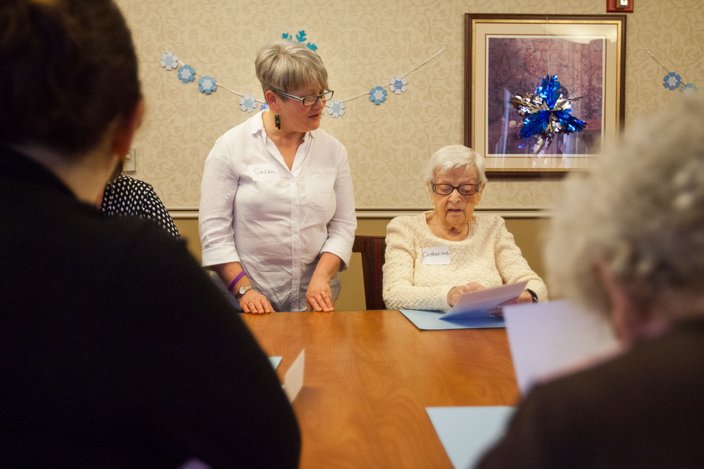January 20, 2014
 Thom Carroll/for PhillyVoice
Thom Carroll/for PhillyVoice
ARTZ Philadelphia Founder/Executive Director Susan Shifrin leads a team of two volunteers in guiding a group of St. Joseph’s Manor Alzheimer’s and dementia residents through a holiday art project. It’s one of several programs ARTZ has taken up.
“Let me show you.”
Edwin traces a watercolor-green Crayola marker around the edges of a slapdash blue circle. With a sudden stroke of precision, he draws alongside its jagged edges until its ends kiss, hanging as a complete unit from a tree branch he scribbled moments earlier. Susan, who stands patiently just over his shoulder, watches in eager anticipation of what he’s trying to show her. Is this it? Might he be remembering something? Everyone else at the table has finished, and all eyes perched at his half wander to him. But just as Edwin lifts the marker off the construction paper with a facial expression of “Voila!”, he pauses and tosses down the marker in defeat.
He’s forgotten what he meant to show her.
It’s a cloudy Thursday morning in December when Susan Shifrin, founder and executive director of art program ARTZ Philadelphia, arrives at the St. Joseph Manor’s Evergreen facility, a care unit for people diagnosed with varying forms of dementia. Shifrin formed the Philadelphia branch of ARTZ, or Artists for Alzheimer’s, in July 2013. The decision to launch came after spearheading an accessibility exhibition and a series of workshops at the Berman Museum at Ursinus College, where she met Sean Caulfield, a co-founder of the first-ever ARTZ program, started in Boston circa 2001. The premise is as simple as the disease in question is complex: Six to 12 people living with dementia gather in a museum or care facility and band together to discuss art or, as is the case this morning, make it. The hope is that through discussion and the study of landscapes, portraits and thought-provoking use of color, memories will swim back to the surface. It’s not an exact science, but there is every indication that it improves behavior, mood and communication and enhances latent cognitive functionality. Shifrin is the fishing rod; the art is the bait; the memories are the fish.
This morning, there are six residents – in mid- to late-stage of the disease, which is not necessarily typical – in attendance, camped out at a table in the Evergreen dining hall, all with glazed-over looks. There’s Catherine, the former Army nurse who still identifies as such; Earhart, the gentle and soft-spoken gentleman in the corner; Flora, the poofy-haired and jolly chatterbox of the table; Fenya, a former teacher whose attention is instantly swept up by a Christmas card Shifrin hands her (“There’s nothing like a handwritten note!” she later exclaims); Mary, whose confused gaze and quivering lip might suggest a later stage of the disease; and, of course, Edwin.
Shifrin begins this morning’s program by instructing the group to look at a picture on the holiday cards she’s distributed among them. It’s a watercolor piece called “Dancing in the Wind,” painted by Chadds Ford, Pa., artist Karl Kuerner. She speaks to them less like dementia patients and more like students.
“OK, boss!” Catherine says.
Shifrin and two volunteer helpers – one a registered art therapist – bounce from person to person, trying to elicit descriptions of the painting that might trigger memories.
Catherine speaks up.
“It looks like snow. In the background, it looks like trees, ornaments,” she says, stringing together her words like beads. “It looks like … Christmas!”
Her face radiates – it’s a moment of realization. If only for a fleeting moment, she remembers it’s the holiday season, and she’s experiencing joy. She’s happy.
It’s been two decades since former President Ronald Reagan announced his Alzheimer’s diagnosis through a public letter. For many people, it finally brought the disease into the public narrative.
“My fellow Americans,” he wrote in November 1994, “I have recently been told that I am one of the millions of Americans who will be afflicted with Alzheimer’s Disease….”
The message was succinct, but the subtext of his language proved remarkably predictive. It turns out, “will be” was an all too accurate choice of words.
Today, more than 5 million people in the United States are living with Alzheimer’s disease; current projections have that number growing to 16 million by 2050, provided a major medical breakthrough doesn’t happen in the years ahead. (It likely won’t; a new Alzheimer’s drug treatment hasn’t been approved for a decade, with modern research mostly focused on unearthing new biomarkers.) Strictly looking at Greater Philadelphia, 158,394 people age 65 and older are living with an Alzheimer’s diagnosis, according to the Alzheimer’s Association's Delaware Valley chapter. That number grows by 10 percent when accounting for people younger than 65. Pennsylvania, which is the sixth most populous state in the country, has approximately 400,000 afflicted with Alzheimer’s as of 2014, according to a Pennsylvania State Plan for Alzheimer’s report issued in February. Thirty-five thousand people died between 2000-10 as a direct result of the disease.
“I don’t know if people realize it’s fatal – they think it’s just something old people get,” says Felicia Greenfield, associate director for clinical and research operations at Penn Memory Center. “And maybe it doesn’t get as much funding as cancer because anyone can get cancer, yet it is the sixth-leading cause of death.”
Newsflash: The population is aging quickly. By 2030, Pennsylvania’s population of those over 65 will increase from 2.7 million to 3.6 million. That’s a 30 percent increase in just 15 years.
In other words, this is everyone’s problem.
Congress has recognized that. At the federal level, funding recently saw an uptick: Congress included the Alzheimer’s Accountability Act in the 2015 budget bill signed by President Obama in December. The Act guarantees federal research, education, outreach and caregiver support each year until 2025. More importantly, it requires National Institutes of Health scientists to re-evaluate the state of Alzheimer’s disease each year and submit new funding proposals to Congress that adjust for up-to-date needs. A sum of $25 million of research funding has been added to the budget for fiscal year 2015, which totals $591 million.
Is this good news? Well, sort of. Scientists estimate that effectively treating Alzheimer’s will require a yearly commitment of $2 billion.
That begs the question: How much money do we allocate to funding an increasingly elusive magic pill, while 5 million people – many of whom, particularly in rural Pennsylvania, lack the resources necessary for constant care -- continue to battle a disease that’s measured not in days, weeks or months, but years.
“These programs make a difference in people’s lives.”
John Zeisel, co-founder of the national ARTZ program and executive director of its parent org, the I’m Still Here Foundation, says this outright. The use of art as a means of treating dementia, Zeisel says, is not at a point of scientific truth – at present, it’s qualitative more than quantitative, though he says the distinction’s often arbitrary.
“It’s just a matter of if you have enough money to count [results].”
But it is part of a larger narrative that begins to address the disease in a way that is not as black and white, doom and gloom, cure or crumble as it is at present.
“If you despair, and take on the point of view that the minute you found out you have cognitive problems is the end of your life, then you’re part of the ‘Despair Narrative,’” Zeisel says. “Thing is, we can get creative about how to engage people with dementia, rather than abandoning them. It’s not, ‘Why bother visiting?’ It’s ‘Visit, and find something to do.’ That’s really a keystone of the ARTZ programs.”
The Department of Neurology at the University of Pennsylvania School of Medicine took a stab at summoning the science of art therapy, publishing a study in the Journal of Alzheimer’s Disease earlier this year that highlights the observed effects of art interaction among Alzheimer’s patients in programs across the country that are similar to ARTZ in how they operate.
“The hardest and saddest part, for me as a caregiver, is watching your loved one’s personality disappear and change to a person who you don’t know. Yet, you love who they were and you love who they’ve become, and together you move forward.”
Here’s the gist of the findings: Art therapy, when structured appropriately, can capture the attention of Alzheimer’s patients; improve neuropsychiatric symptoms, self-esteem, social behavior and – the real kicker – provide pleasure. Why? And how? People with early Alzheimer’s disease encounter short-term memory problems that extend to parts of the brain concerning language and spatial reasoning – basic communication and judgment, in a nutshell. But what they don’t lose is vision, sense of touch or basic coordination; that, combined with the preservation of “procedural memory” (the motor memory that allows us to ride a bike without face-planting on the pavement), allows art to interact with the brain because it doesn’t necessarily require personal memories or traditional language channels. They’re living in the moment, with the potential to reach into their past. To boot, the research suggests that patients’ ability to enter a flow state – the ultimate indicator of well-being (pleasure) – is also intact when discussing or making art.
Basically, art acts as an arbiter: It’s the preschool teacher pointing kids to their latent ability to comprehend and express the rhythm and rhyme of their ABCs, rather than the haphazard implications of their triangle house and stick-figure family – only in reverse. It’s art as language.
“You’re in a situation where you’re capitalizing on what’s preserved, rather than having patients keep facing where they have their problems,” says Anjan Chatterjee, a professor of neurology at the University of Pennsylvania and co-author of the study. “You can think of it as a model of intervention that’s not trying to compensate for someone’s deficits, but trying to enhance and preserve what people can do. It gives them a vehicle for communication to be able to express some of their rich, interior emotional lives that they can’t express in language.”
In that sense, it’s invaluable for the caregivers (669,000 in Pennsylvania, as of 2013) who also deal with this disease – both financially and emotionally – and yearn to understand the transformed version of loved ones, or at least tap into their former selves for a moment in time.
“Every day, your loved one is changing as dementia takes a stronger hold on their daily functioning,” says Nancy Hays, a registered art therapist who graduated from Drexel University’s art therapy program and volunteers for ARTZ Philadelphia. A close family member was diagnosed with early onset Alzheimer’s disease in 2007; she brought him to one of the first ARTZ museum groups, thrilled to have found “something to do” with him – a means of connection.
“The hardest and saddest part, for me as a caregiver, is watching your loved one’s personality disappear and change to a person who you don’t know. Yet, you love who they were and you love who they’ve become, and together you move forward.”
Currently, little of the quantitative research Zeisel referenced is being done, but that’s largely because the efficacy-affirming money just isn’t there. It’s a circular problem: Researchers won’t study it because they don’t have funding, but funders won’t funnel money into a research area that hasn’t shown numerical promise.
“The roadblock for a research program like this is funding,” Greenfield says. She’s set to coordinate with Shifrin later this month to discuss a partnership that would include ARTZ participants in a formalized study conducted by the center. They hope to find a foundation to fund the project. Greenfield expresses further frustration that her organization’s operations are so dependent on NIH. “I really feel as though Medicare and insurance providers should provide [support].”
The problem, Chatterjee says, is that the hard data has yet to be set in stone that will convince insurance companies and Medicare to pay for art therapy.
“Often, people think of [art therapy] as ‘soft’ – it’s hard to control,” he says. “People who have direct experience with individuals with Alzheimer’s disease have this intuition that patients enjoy doing art and is a way to communicate with patients, but it’s hard to back that up with randomized controlled trials, which show where the efficacy is.”
What the Penn Memory Center needs, then, is an outside advocate and figurehead.
Enter: Susan Shifrin.
I first meet Shifrin at the Barnes Foundation for a run-through of what she ordinarily shows her ARTZ groups. She’s planted on a bench, gabbing with a Barnes employee about her program. She has short, wispy gray hair, a yellow scarf that drapes to her knees, a black-leather pocketbook and rectangular frames with teal-colored arms that stop them from being ordinary. Her speaking tone is defined by the seesawing inflection of her voice – at one moment a whisper, at the next a dramatic and animated whisper-shout that sounds like a librarian reading a fairytale to schoolchildren.
That her profession is museum curating would come as a shock to … no one.
Shifrin grew up in Boston before attending college at Yale and Brandeis. She moved to Philadelphia in 1989 for Bryn Mawr College’s master’s program in art history (she would later get her doctorate from there). Her father was a composer, her mother an aspiring pianist.
“I’ve always been in the arts,” Shifrin says. “There’s art in my blood.”
Her fascination with museum curating and education stems from her interactions with a costume designer and historian at Brandeis, who led her to a job as a department assistant in costume and tech at the Boston Museum of Fine Arts in 1984. That’s when she started to make sense of her fixation on museum work.
“It has to do with the personal components of it – people wear costumes, people use textiles….” she says. “That was the start of my interest in people and objects and how they intersect.”
Her interest in that intersection came to a boiling point while working at the Berman Museum at Ursinus and sitting in on conversations about accessibility. She would observe accessibility programs for the blind and wheelchair-users and was floored that those with dementia – dubbed a niche group by many museums, despite the disease's prevalence – were left in the dark.
For her, it felt personal.
Her mother was diagnosed with Alzheimer’s in 2000. Shifrin has seen its ups and downs and empathizes with – has adulation for, in fact – the caregivers who accompany loved ones for her tours; caregivers who, in reality, battle the disease as much as the person with the diagnosis, experiencing their own health struggles as a result of stress.
“This sounds terrible, but I feel like it’s important that I was one of those caregivers who was terrified by the disease – terrified by what I saw it doing to my parent, who would have happily dug a hole in the sand and put my head in it,” she says. “Because I think, as sad as it makes me now, all the opportunities I missed, it also means I can understand much more readily what the caregivers we work with are going through. And I think that, as much as ARTZ is about creating safe, productive and engaging spaces for people with the diagnosis, it’s also about creating safe havens and respite – places of understanding for caregivers, too.”
In which case, she’s re-thought accessibility in a way many museums have yet to do. She’s started with the Barnes and Woodmere museums as locations for her program but plans to expand into three more regional museums in 2015. She hopes to offer a program every week by Summer 2015.
“This isn’t about [reaching] people who happen to have disabilities,” Shifrin says. “This is about reaching everyone – through so-called ‘accessibility programs.’”
So, when she’s not doing private ARTZ programs at facilities like Evergreen, she’s facilitating open-to-the-public discussion groups at places like the Barnes – a museum particularly notorious for its placement-as-storytelling artwork.
“Enough research has been done to know that narrative works – ones with landscapes, people, townscapes. That kind of genre with the underlying possibility of storytelling tends to be most powerful,” Shifrin says, as she stands before Seurat’s “Models” and Cezanne’s “The Card Players.” “Once I’ve [determined what to show], my next thought is, ‘What kind of connections can I tease out of them?’”
“I have had the privilege of witnessing people seemingly find themselves again. And that is the incredible power of this,” Shifrin says.
Indeed, her program is like a Socratic method for Alzheimer’s. She pinpoints parts of a painting that might spark discussion and tethers participants together through chitchat. Shifrin is clear that she is not a registered art therapist, but that the program is a gateway to art therapy and shares its core fabric. ARTZ will offer an art therapy course in Spring 2015 in association with the Pennsylvania Academy of the Fine Arts. It will be taught by registered art therapist Dona Duncan.
“[With my class], they’re able to block out other thoughts and feelings and are able to be in the moment with what they’re doing,” Duncan says.
The formalized therapy exercises combine yoga, visualization techniques, art-making and observing.
“That can jar memories – seeking a picture of a memory, or drawing it. And while they’re doing that, they’re relaxed; they’re not tense. They’re not being judged or afraid to make a simple mistake. And when they have that experience, they feel so good about themselves, and they don’t feel isolation – and that, the isolation, that’s the worst form of pain.”
Alzheimer’s patients are as much victims of their mental impairment as they are of basic neglect, not always at the fault of caregivers or medical practitioners.
“They rarely have someone who just sits down and talks to them,” says Sue Brown, who volunteers with ARTZ as well as the Alzheimer’s Association’s “Memories in the Making” program. “And that’s where the change comes in: When they can be heard.”
This, as one might imagine, is where money might come in handy – if not to research and fund programs like Shifrin’s, then to at least ensure patients more opportunities to be wheeled away from the window or television set and offered – not forced into, per se – social outings.
“The internal experience of various kinds of dementia is an alienating one to begin with. So, put that together [with being isolated in an unfamiliar care facility], and you have people who become non-communicative; they become totally turned in on themselves, and it’s hard to connect,” Shifrin says. “It’s particularly hard for families to connect, because they see what isn’t there anymore first and foremost. Part of the theory of what we’re doing, and what other organizations around the country are doing, is giving people the opportunity – if they want it – to focus on something outside themselves.”
In essence, it’s an opportunity to remember – to experience social engagement and dust off the cobwebs in parts of the brain that have lost their shine, not their sustenance.
“I have had the privilege of witnessing people seemingly find themselves again. And that is the incredible power of this,” Shifrin says. “A father may not remember his daughter’s name anymore, and that’s devastating, but that doesn’t mean he doesn’t remember her. He may not remember what role she played in his life, but he remembers he has a close connection with her. … An advantage to this work is we see them now and appreciate who they are now; we’re not plagued by what they used to be.”That much hints at the overall message: This isn’t a pity party, or a means for Shifrin to clear her conscience; quite simply, it’s a way to brighten someone’s day – to give people with dementia the quality of life that the front pockets of the science community and money-handlers have seemingly told them they can’t have.
“This is not just a ‘mission of mercy,” Shifrin says sternly. “It’s a mission of respect and appreciation and, acknowledging that, as devastating as these illnesses are, they come with some kind of inadvertent side effects.”
“And sometimes,” she adds, “those side effects are wonderful.”
Shifrin and Brown are huddled with Edwin and are talking him through childhood memories of dreidels. Shifrin feels silly, not having realized that some of the residents might be Jewish (three of the six, as it happens) and not relate to the Christmas painting she’s brought. But that the conversation about the holiday season is happening at all, she recognizes, is something of a blessing. Because of it, Hanukkah is Edwin’s “right now” – one of many snowflake “right nows” he’ll experience as his disease progresses. The conversation they snowball into has nothing to do with the painting in front of them, but that’s exactly the point: Unfurling the tightly wrapped personal identifiers that have been sealed away for years, bringing consciousness to a place of serenity. Edwin’s telling a story, brought on by whatever tale the painting happened to be telling through his eyes.
Mary, all the while, is sitting across from him, visibly having trouble unpacking what’s playing out before her. She’s unresponsive – the most anyone can get out of her, in this particular moment, is a “Yes” or “No.” Her bottom lip continues to quiver; she hesitates when the others start drawing and stares off blankly.
Hays quickly notices the disconnect and comes to her aid. She eases the brown marker into her hand and assists Mary in guiding it across the paper.
“That’s a good start, Mary! Wonderful!” Hays says.
Hays steps away for a moment, and Mary instantly recedes back into her disease. She’s staring off again, but this time, she is scanning the crowd for understanding – appearing to desperately want a fuller comprehension of what she’s doing and why she’s there. Her head tilts in all directions as she observes the ruckus: Fenya, to her left, is gluing ornaments on her paper with a pounding of her fist, like she’s stomping out a fire with her boot; to her right is Earhart, proving remarkably receptive and energized as he signs his picture (a few illegible letters and a curvy scribble); Catherine, meanwhile, cherry-tops her work with a few finishing brushes – she is the apparent Picasso of the bunch.
And there’s Mary … staring.
“Will I get money for this?” chirps Flora in the background, amidst the hoopla (she’s serious).
Laughter ensues.
And there’s Mary … staring.
By the time the hour’s over, Mary has a fully stocked picture to call her own – it requires some cajoling from Hays, but she’s done it. Scrawled green and brown lines, pink and glittering white ornament cutouts – she’s not created the "Mona Lisa," but, again, she’s done it.
“Good job, Mary!” Hays exclaims.
Mary half-smiles. It’s the most her muscles have stretched all morning. Then she starts staring again, first at her faded pink nails, but then at her picture.
She turns to Hays before being wheeled over to the corner of the room.
“Thank you, hun,” she says, gratitude dripping from each word.
… And then she’s back to staring – once more, at her picture. Her eyebrows furrow, and for the first time, the quivering stops. She’s waiting for something. Whether she’s waiting for someone to wheel her back to her room, for a memory to come back to her or for someone to make her a sandwich, is a mystery. But for the moment, mesmerized by her picture, Mary has an identity. She’s Mary, the artist, and not Mary, the person with dementia; she’s Mary, a person who draws, who has friends, who just received a holiday card, who just so happens to have dementia.
Just then, the activities director comes from behind to wheel her off to the residential wing. But as she rolls away, I catch one more glimpse of her face. Glued on it: a smile.
She’s happy.