
July 12, 2016
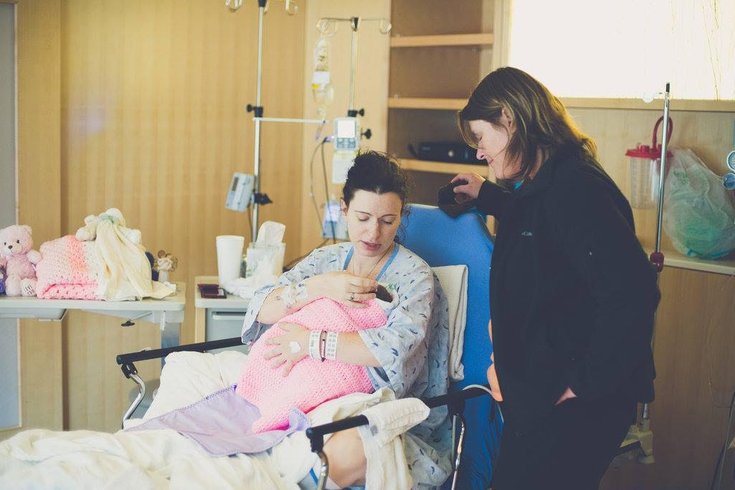 Kim Rodgers with Brinkstreet photography/for PhillyVoice
Kim Rodgers with Brinkstreet photography/for PhillyVoice
Bereavement doula and author Elizabeth Petrucelli supports a mother after loss.
Midway through an evidence-based and heartfelt training on pregnancy loss, we take a break.
“Get outside, go for a walk, get some tea, stretch,” I say while introducing a 15-minute hiatus from a difficult topic. “Take care of yourself.”
I organize my notes and breathe deeply. Conversation fills the room. The 25 or so individuals gathered – midwives, nurses, lactation consultants, therapists, OBs and doulas – enjoy a short respite.
As I fill a cup with hot water for tea, a young doula approaches me.
“Stillbirth scares me,” she confides. “I know I’ll encounter it at some point in this work and that scares me.”
“I hear you,” I state, nodding my head.
“But you know what?” she continues. “The whole idea of companioning helps. It really does. I don’t need to be an expert. I don’t need to fix the situation. Mostly, I just need to show up with love and courage.”
“I believe you can do that.”
“Yes. I can.”
Today, more and more American women are hiring birth and postpartum doulas to offer support, guidance and companionship through labor, delivery and the postpartum period. Originally a Greek term for women servants who attended laboring mothers, the word “doula” has entered our common lexicon.
But the role of a doula is changing. Doulas are no longer associated only with birth and/or infant care. The comfort measures and care practices that doulas bring to the beginning of life now are being applied to life’s end. While still in its nascent stages, there is a growing movement to train end-of-life doulas, abortion doulas, loss doulas and death doulas.
Whether holding space for birth or death, doulas offer compassionate companionship through our most challenging and meaningful transitions. Doulas work in threshold spaces and support individuals as they journey from the known to the unknown, from one stage of life to the next.
For expectant couples facing miscarriage, stillbirth and/or infant loss, the journey is often terribly difficult.
Tara Nichols remembers how it took years to find parts of herself again.
“My own experience with the loss of a baby was that others expected my grief to be brief because he was only here for a brief time,” she recalls. “The general consensus seemed to be that I should be able to 'get over it' or 'move on' quickly. However, I felt like my world shattered.”
In 2012, Nichols lost her son Maxwell due to a congenital diaphragmatic hernia. Nichols and her husband exhausted every option in the hope of saving Maxwell’s life. Their efforts, combined with the determined efforts of medical personnel, sadly could do nothing but “prolong the inevitable.” A palliative delivery was planned. Maxwell lived for one hour.
The resulting emotional devastation was profound. How to make sense of Maxwell’s death? How to live with such immense grief?
Nichols remembers: “One of the best pieces of advice that I got from a fellow bereaved parent was the permission to just be. To stop looking for my old self because undoubtedly this experience would irrevocably change me … and that was OK.”
The companioning model of caring for the bereaved powerfully affirms the wise advice offered to Nichols. This model of care is the brainchild of Dr. Alan Wolfelt, director of the Center for Loss & Life Transition. According to Wolfelt, our contemporary understanding of grief is distorted. Too many of us approach grief as an illness to be cured, something to be fixed or something to overcome. The goal is to put the loss behind you and return to the normalcy of one’s prior life. Due to this “managed care” approach, Wolfelt argues that we forget there are “more life-giving, hope-filled models that incorporate not only the mind and body, but the soul and spirit.”
In a keynote address entitled “Companioning vs. Treating: Beyond The Medical Model of Bereavement Caregiving,” presented for the Association for Death Education and Counseling, Wolfelt offers insight that is particularly helpful for doulas to remember when encountering pregnancy loss.
He states: “To heal in grief one must turn inward, slow down, embrace pain, and seek and accept support.” Furthermore, “we as human beings are forever changed by the death of someone in our lives.” Honoring this change, rather than trying to treat, overcome or fix it, is central to the task of companioning.
When a baby dies in labor or after delivery, tears and shock usher forth. It’s one thing to companion a mother through the grueling physical demands of birth – hour upon hour, comforting through the waves of contractions. It’s quite another to do this work and then watch a mother hold her beloved dying or deceased child to her breast. The new doula that approached me during our training break isn’t the only one who feels afraid. How can we best support a mother through such profound anguish?
It behooves doulas to prepare. Despite our fears, we must ask the above question. Consider that 1 in 4 or 5 pregnancies end in miscarriage. One out of 160 births in the United States end in stillbirth, and the rate of infant mortality in this country is far too high. The Centers for Disease Control and Prevention reports that 25 nations have lower infant mortality rates than we do.
In our training, I highlight a number of practical “care practices” that one can employ in order to strengthen circles of support following pregnancy loss. For example: What activities/rituals can bring needed comfort to the mother, her husband/partner and the immediate family? How can we work with hospital staff to ensure that protocols regarding perinatal loss are sensitive to the needs of bereaved parents? How can friends and community members extend their love and sympathies in helpful ways, avoiding well-meaning but hurtful words? Are we familiar with legal options that exist with regard to caring for the deceased baby’s body? What do we know about alternatives to embalming or autopsy? What do we know about home funerals? And last but not least, how do we, as care providers, care for ourselves?
These are all important questions to consider. Most importantly, however, doulas of birth and death can draw upon the wisdom of companioning in supporting devastated families to turn inward. We can hold space as they embrace the grief of a little one’s death. And we can do our humble best to show up with a courageous, quiet, gentle and loving heart.
“It was the rare few who were willing to bear witness to our pain, memories and love,” Nichols laments. Those of us teaching doula care practices to best support both the birthing and dying are working to change that.
Learn more about the work of bereavement doula and author Elizabeth Petrucelli. You can also learn more about Holding Space for Pregnancy Loss trainings offered by PhillyVoice.com contributor Amy Wright Glenn.
Interested in Amy Wright Glenn's work? Sign up for Amy's email newsletters today.
Follow Amy on Twitter: @amywrightglenn
Add Amy’s RSS Feed: Amy Wright Glenn