
May 14, 2021
 Courtesy/Fred Rahmanian
Courtesy/Fred Rahmanian
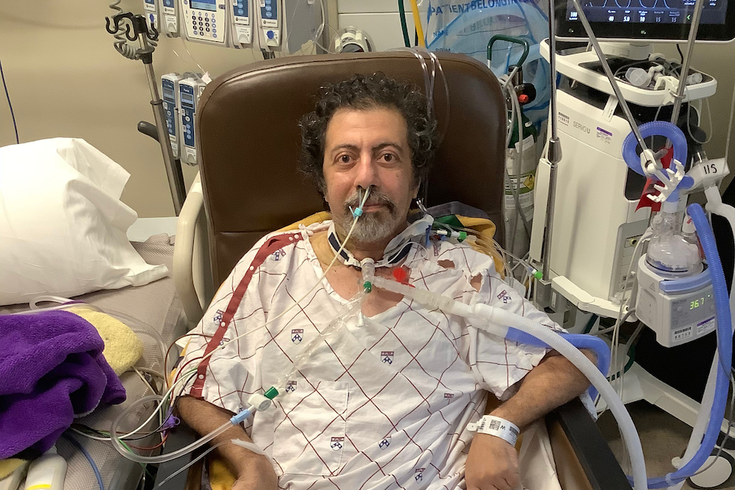
Fred Rahmanian says he was determined to return to his Berks County home as soon as possible after his double-lung transplant. He wanted to provide 'some sort of normalcy' to his family after months in the hospital.
Fred Rahmanian faced an immense decision when he was brought out of sedation at the Hospital of the University of Pennsylvania last December.
Rahmanian, 54, had spent weeks on life support amid a battle with COVID-19, but his failing lungs had not shown any improvement and he was out of treatment options. His only chance at survival was a double-lung transplant, his doctors explained.
"They told me you have to consent to this, this is the last option," said Rahmanian, of Bern Township, Berks County. "There's nothing left. You're going to expire, you're going to die."
To Rahmanian, this initially sounded incredulous. Hadn't he just been admitted to Reading Hospital with a fever and a bad cough?
He didn't realize that he had spent nearly two months attached to a machine that had taken over his lung function. He did not know that he had coded during his transfer to Penn Medicine, nor that he had overcome a life-threatening case of sepsis. And he had no idea the lengths that his wife, Pam, and others had gone to support him.
"They were trying to explain to me that it was more than two months since then and I just didn't remember any of it," Rahmanian said. "That's when it dawned on me that I'm getting very close to the end. And that's where there are all these thoughts that go through your mind."
Rahmanian wanted to see his triplets — Cyrus, Darius and Maryam — turn 18 in February. He wanted to see them graduate high school and head off to college this fall. And he wanted more time with Pam.
Only a handful of COVID-related lung transplants had been conducted in the United States at the time — none of them in Pennsylvania. On Jan. 1, Rahmanian became the first.
At the beginning of the pandemic, health systems didn't anticipate COVID-19 patients would prompt a great need for lung transplants.
Hospitals operated on the assumption that most COVID-19 patients would recover organ function on their own, or die of complications before a transplant became a possibility. Plus, the initial surge required such resources that hospitals merely focused on keeping patients alive.
"The reality is that transplant is reserved in very selected options for patients with advanced lung condition," said Dr. Christian Bermudez, director of Penn's thoracic transplantation. "We were concerned that the number would be so overwhelming and that patients would be so sick that none of them would get to transplants. And we were wrong."
The coronavirus has left thousands of U.S. patients with badly-damaged organs. Many of them have developed acute respiratory distress syndrome – a condition in which fluid develops in the lungs' air sacs – or pulmonary fibrosis, the scarring of lung tissue.
As as a result, transplants are becoming increasingly common among COVID-19 patients with irreversible lung damage.
Nationwide, there were 26 patients on waiting lists for COVID-related transplants as of Wednesday, including two in Pennsylvania, according to the United Network for Organ Sharing, the nonprofit that manages the U.S. organ transplantation system.
At least 112 COVID-related lung transplants have occurred in the United States through April 30 – and nearly half of those have been performed in the last two months. There also have been four heart transplants and one heart-lung transplant.
Nearly 40 U.S. hospitals have performed COVID-related transplants. In the Philadelphia region, Penn Medicine has completed five lung transplants; Temple Health has done four. And they expect to do many more over the ensuing months.
Dr. Christian Bermudez
"The reason why we're doing more transplants now than before is that ... we're just about seeing the long-term problems that COVID can cause in the lungs," said Dr. Sameep Sehgal, a pulmonologist at Temple. "Secondly, we have more resources available at this phase of the pandemic than we had last spring, which may have an effect on how many patients we're able to see for transplant evaluations."
(Read about one of Temple's patients who received a single-lung transplant in March.)
Several months into the pandemic, Penn Medicine began placing severe COVID-19 patients on ECMO machines — a life support technology that pumps blood from the body, oxygenates it and returns it to the body. The machine provides the failing lungs a chance to heal. But that's no sure thing.
Only about 50% of COVID-19 patients placed on ECMO survive, Bermudez said. Many succumb to infections, bleeding complications, strokes or multiple organ failures. Some, like Rahmanian, never regain their lung function but become candidates for transplantation.
"To be able to save at least a few of them, especially young patients with families, it is really gratifying," Bermudez said.
But initially, there was no roadmap for them.
Hospitals were wary of the COVID-19 risk a transplant might pose to medical personnel. There were questions about whether patients could survive the surgery. And guidelines dictating eligibility needed to be ironed out.
Penn is limiting COVID-related lung transplants to acute patients who are younger than 60 and have been on ECMO for at least four weeks – enough time to allow the lungs to recover on their own. Eligible patients must no longer be transmitting COVID-19, cannot have any other organ failure and must be interactive. That's in addition to the standard transplant qualifications.
Temple has adopted similar guidelines.
"Lung transplants are great options for patients in advanced lung conditions, but it's not a cure," Bermudez said. "So we really try to reserve lung transplants for patients that are not recovering."
Fred Rahmanian spent more than six weeks on ECMO, a life support system that takes the function of the lungs, amid a life-threatening battle with COVID-19. He underwent surgery for a double-lung transplant on Dec. 31, 2020.
Pam Rahmanian got the call not long after she arrived at work on Nov. 9. The news was grim: her hospitalized husband had taken a turn for the worse.
The coronavirus had made its way through the Rahmanian household in late October. For Maryam and Darius, it was like a bad flu. Cyrus never tested positive. The virus briefly hospitalized Pam, but by this point Fred had spent nearly two weeks in the hospital.
Now, out-of-state family members were headed to Pennsylvania expecting to stay through Fred's funeral. His medical providers wanted to intubate him and his brother — who serves as his primary care physician — was urging him to allow it. Meanwhile, his boss at Capital Blue Cross was busy helping Pam seek a transfer.
"That's when it really, really hit me that he's seriously ill and he may not make it through this," Pam Rahmanian said.
Two days later, Penn's Lung Rescue Team arrived to rush Fred to HUP. Patients typically are airlifted, but a raging storm had made helicopter travel unsafe. So the team transported Fred via ambulance, placing him on a mobile ECMO unit. Along the way, he coded and needed to be revived.
At Penn, Fred was given up to six weeks on ECMO. The hope was that his lungs would begin to heal within that timeframe. If his lungs hadn't shown progress by then, his only hope might be a transplant – but Penn had yet to perform one on a COVID-19 patient.
It was pretty awesome and pretty unusual that you could say the surgery started at 11 p.m. on New Year's Eve and it finished on New Year's Day." – Pam Rahmanian
"The challenge with Fred was to what extent we would wait to allow the chances of the lungs to recover," Bermudez said. "That is not well defined. We have learned from other viral infections that, in general, you can expect recovery within two or three weeks, or up to a month. ... In Fred, we were six, seven weeks out."
Thanksgiving came and past. Along the way, Fred survived a case of sepsis. But by mid-December, Fred's lungs were not doing any better. And his doctors did not expect him to show any improvement.
"You can imagine the whole time you're on pins and needles," Pam said. "Now, they're telling you it's almost certain that your husband is going to pass away. I'm going to say that that is probably the first time that I became a basket case and was for a couple of days."
Three days later, Pam received a call that offered a glimmer of hope. Penn wanted to pursue a transplant.
Pam immediately agreed, and Fred was tested to determine if he would qualify. His lung allocation score was so high that it catapulted him to the top of the transplant priority list, and it also further illustrated the direness of his situation.
Pam enlisted her church, school and others to pray for Fred – as she had throughout the ordeal.
"I was having constant emails and texts going out to people saying, 'Please pray that we are able to find new lungs and if new lungs are found, please understand that someone is giving up their life and pray for that person's family, as well."
Within 72 hours of being placed on the transplant list, a matching set of lungs had been found. Fred underwent surgery late on New Year's Eve.
It was a long night, full of uncertainty. Pam stayed up until 2 a.m. before she turned in, figuring no news was good news. Her daughter had a friend over. Her sons passed the time playing video games.
Bermudez finally called at 5:15 a.m. Pam answered before her phone had finished its first ring: The surgery had been successful.
"It was pretty awesome and pretty unusual that you could say the surgery started at 11 p.m. on New Year's Eve and it finished on New Year's Day," Pam said. "So truly, he was given a new lease on life in a new year, which is just amazing in itself."
Fred Rahmanian had lost 50 pounds prior to receiving a double-lung transplant. Several months after the surgery, he is still working to regain full strength.
The path that COVID-19 patients have taken to lung transplantation differs from what is typical.
"Most lung transplants that we do are for patients who have severe lung disease for a long period of time and are usually at home when they're called in for transplants," Sehgal said. "While they are chronically sick, they are not acutely sick in the ICU or have not been in the hospital for weeks when they actually undergo the surgery."
The weakened condition of COVID-19 patients increases the risk of their transplant procedures – their failed lungs can be more difficult to remove from the chest cavity and there's a higher chance of bleeding, Sehgal said. And their de-conditioned states can make recovery much more difficult.
Dr. Sameep Sehgal
Both Sehgal and Bermudez anticipate the COVID-19 pandemic will increase the need for lung transplants. Not only will there be acute patients in need, but others who endured lung injuries may need them down the road.
"We're expecting this number to grow, especially in the next year, year and a half," Bermudez said.
There have been more than 44,200 lung transplants completed in the U.S. since 1988, according to the Organ Procurement and Transplantation Network. More than 600 have been completed this year, a total that aligns with the pace seen in recent years.
The one-year survival rate for single-lung transplants is about 78%, according to the National Hart, Lung and Blood Institute. About 51% of transplant recipients live at least five years. The survival rates for double-lung transplants are slightly better.
It remains to be seen how well patients who needed COVID-related transplants will fare. But early data has doctors optimistic, particularly since they are being performed on patients who have spent months in the intensive care unit.
"We were expecting higher mortality, but so far the mortality seems to be comparable to other similar sick patients in the ICU waiting for transplantation," Bermudez said.
One recent study examined 12 of the first double-lung transplants performed on COVID-19 survivors in the U.S., Italy, Austria and India. As of mid-April, 10 of the recipients had survived and were doing well. The study's co-author separately reported that the first 50-plus transplants in the U.S. also were still alive.
Yet, the longer-term effects and the potential for chronic rejection in COVID-19 patients remain unknown.
"Those things have yet to be defined," Bermudez said. "We'll just know as we try to rescue some of these patients."
Fred Rahmanian, center, enjoys a meal with his family prior to his battle with severe COVID-19, which necessitated a double-lung transplant at Penn Medicine. Clockwise from top left: His sons Darius and Cyrus, daughter Maryam and wife Pam.
Fred Rahmanian was out of the hospital in time to celebrate his triplets' 18th birthday on Feb. 18.
Getting there was no small feat.
After the transplant, Fred expected to spend 6-8 weeks recovering in the ICU before another 2-4 weeks at a rehabilitation hospital. He was out of the ICU within three weeks and released from the rehab hospital after 10 days.
"When I was in the hospital, I had pictures of my family posted right in front of me," Fred said. "Every time I opened my eyes, that's who I saw. They were my inspiration. ... I was determined to get through this successfully and be home and provide some sort of normalcy."
Fred lost 50 pounds while lying in the hospital. His muscles were so weak that he couldn't even turn a doorknob, let alone walk on his own. And he needed to adapt to breathing without a tracheostomy.
"When I came out of surgery, I couldn't talk any more because I had a trache," Fred said. "Imagine being in the ICU, almost a paraplegic. I can't do anything. And I can't talk, but then you have to interact with them, so it was very hard. So my goal was to get to a point where I could talk."
I don't know how much longer I'm going to be here, but at least I made it back. I'm home now. That's a big deal. – Fred Rahmanian, COVID-19 survivor
Fred also developed an infection that proved resistant to all but two antibiotics. His doctors put him on an inhaled version of one of them and his infection cleared up. But it underscored the fragile immune system that transplant patients endure.
Lung transplant patients are given three drugs that suppress their immune response and prevent their bodies from rejecting their new organs, said Dr. Sarah Longworth, assistant director of Penn's transplant infectious diseases program.
"Any type of infection could cause a problem," said Longworth, who treated Rahmanian. "Lung transplant patients are certainly at more increased risk for pneumonias than other transplant recipients, but any infection could have a more severe outcome compared to normal, immunocompetent hosts."
The pandemic only heightens that risk, Longworth said. Penn is counseling all of its transplants to be vigilant about their social distancing and hand hygiene – even those who previously had COVID-19.
After his release from the rehab hospital, Fred spent another three weeks living with his family at a hotel in Malvern – Penn requires transplants patients initially stay within an hour of Philadelphia. In late February, he finally returned home.
By then, Pam had begun filling him in on the details of his journey. He had gained a deeper appreciation for the widespread support his family received and for Pam's dedication.
"I felt that I had two miracles," Rahmanian said. "The first miracle was my wife and the second one was my lungs. Without my wife, I wouldn't be here. She managed to work, she managed the household and she managed me."
Pam credits her religious faith, specifically the power of prayer, for instilling a sense of calm throughout the ordeal.
"It's what brought me through," Pam said. "It's what brought my husband through. It's what brought this family through, along with everyone else I had behind me supporting me – and there was a lot. I'm eternally grateful to everyone who did help and continues to help."
Rahmanian still requires help getting around the house. He still gets fatigued. And he's on a litany of medications. But he is back working part time as a data scientist and he plans to finish up his doctorate degree at Drexel University.
Most importantly, he is home.
Pam quietly snapped a photo of Fred sleeping next to her that first night, grateful for more time with her husband. Fred has enjoyed watching his kids go about their days and playing with the family dog. Even just sitting in his own chair carries emotional weight.
"It's just that feeling of I'm home now," Rahmanian said. "I've made it through all of that ordeal. I don't know how much longer I'm going to be here, but at least I made it back. I'm home now. That's a big deal."
 Source/Penn Medicine
Source/Penn Medicine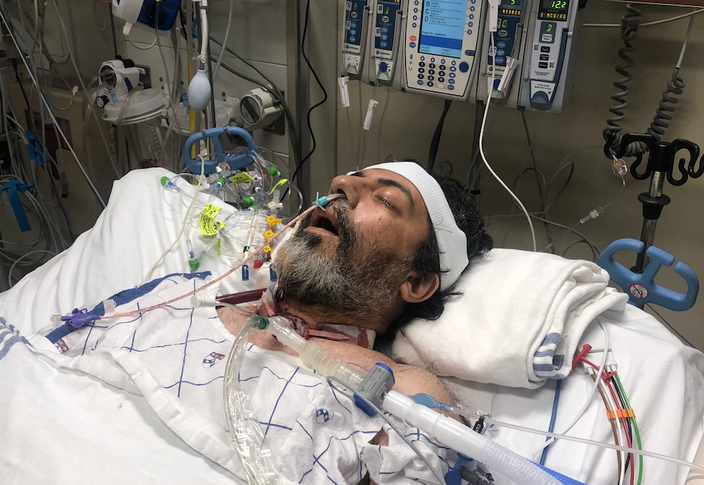 Courtesy/Fred Rahmanian
Courtesy/Fred Rahmanian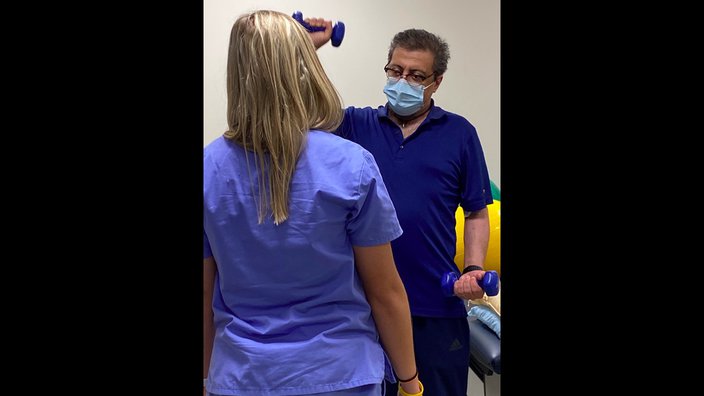 Courtesy/Fred Rahmanian
Courtesy/Fred Rahmanian Source/Temple Health
Source/Temple Health Courtesy/Fred Rahmanian
Courtesy/Fred Rahmanian