
September 26, 2018
When it comes to your skin, getting older isn’t all bad news. Older people heal skin wounds with thinner scars.
As a practicing dermatologist, my physician colleagues and I make this somewhat counterintuitive observation routinely. But how this occurs is not well understood. Mailyn Nishiguchi, a graduate student, Casey Spencer, a research technician, and I worked together to discover how aging normally modulates how our skin heals and the thickness of our scars.
RELATED READ: Why losing a dog can be harder than losing a relative or friend
My laboratory at the University of Pennsylvania studies how to heal human tissues without a scar. Organisms heal skin wounds using two different processes: scar formation and tissue regeneration. Tissue regeneration results in the return of the original tissue architecture and absence of scars. Scar formation results in fibrous tissue deposition that obliterates the tissue architecture, and generates a thick line of raised red skin. Mammals generally repair injured tissue with scar formation.
In experiments we observed that when young mice were injured, they healed with a scar. However, when elderly mice were injured, their skin wounds regenerated and repaired without a scar. These results reflected what we have observed in our clinic patients. We concluded that aging improves tissue regeneration in both mice and humans, and we set out to understand how this works.
First, we wanted to see if this change was due to a circulating factor in the blood. We exchanged blood between young and old mice through a technique called parabiosis. When elderly mice were exposed to young blood, their skin no longer regenerated as well. Thus, young blood contained a circulating chemical that promotes scar formation and prevents tissue regeneration from occurring.
To identify this factor, we compared gene activity between injured young and elderly human skin. We focused only on the genes of proteins circulating in the blood and found 13 different proteins in old versus young skin. One of them, SDF1, had previously been shown to regulate tissue regeneration in the skin, lung and liver.
Older mice heal skin injuries without a scar.
To prove that SDF1 may be the mysterious factor responsible for scarring in the young animals, we engineered a mouse that lacked the SDF1 protein in the skin. When SDF1 was eliminated, young mice regenerated their skin with no scarring, just as in elderly mice. Therefore, we concluded that SDF1 promotes scar formation in young mice.
How does getting older shut off SDF1 production? We discovered that a different protein, called EZH2, turns off the SDF1 gene, and as mice aged, the amount of EZH2 rose. To take this one step further, we used a drug to block EZH2 function in elderly mice. In the absence of EZH2, elderly mice reactivated SDF1 and lost their ability to regenerate their skin.
We wanted to see if these findings also held true in human skin. Similar to mice, skin injury in young people triggered SDF1 production, and this induction was diminished in elderly human skin. We also showed that EZH2 is the reason behind this change. In this case, mouse and human skin behaved in the same way.
Why do mice and humans form more scars when they are young? We speculate that this is a trade-off between speed and quality. Tissue regeneration is a slow process – it takes a month for our skin injuries to regenerate. Meanwhile, a scar can form in little as three to five days. As a young animal, one would want an injury to heal as quickly as possible to live to fight another day. You will tolerate imperfect healing for a faster response. Whereas, older animals that have passed their reproductive prime may not need to heal as fast.
Taken together, we identified a rare example where aging improves tissue function, specifically the tissue repair process. We are planning a clinical trial with the drug, plerixafor, an existing FDA-approved SDF1 inhibitor which is currently used to mobilize stem cells for bone marrow transplant patients, to test its efficacy in preventing scar formation in humans.
Currently, there are no effective treatments on the market to prevent scar formation. In addition to scars from acne and incidental trauma, we hope this approach may be beneficial for many types of human tissue injuries, including the genetic disease epidermolysis bullosa, an extremely debilitating blistering skin disease, in burn patients, or patients with keloid scars.![]()
Thomas Leung, Assistant Professor of Dermatology, University of Pennsylvania
This article is republished from The Conversation under a Creative Commons license. Read the original article.
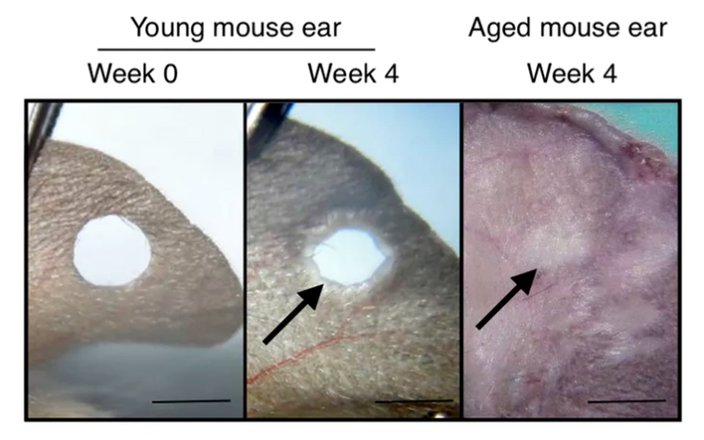 Thomas Leung/CC BY-SA
Thomas Leung/CC BY-SA