
March 02, 2020
 Hans Braxmeier/Pixabay
Hans Braxmeier/Pixabay
Psoriasis is a common skin condition that causes raised, red, scaly patches of skin that can turn itchy or painful. In the most severe cases, it can lead to joint disease or permanent disfigurement.
Psoriasis is a common skin condition that causes raised, red, scaly patches of skin that can feel itchy or painful. But if that inflammation can't be kept in check, it can affect a person's entire body.
Psoriasis prompts skin cells to rapidly multiply, causing a buildup of lesions on certain skin surfaces. Many cases are mild, but severe cases can lead to permanent disfigurement and joint disease. About 30% of people with psoriasis will develop psoriatic arthritis, which causes inflammation in the joints and tendons.
The condition's pathology is not really known, according to Dr. Jonathan Wolfe, head of the dermatology division at Einstein Medical Center Montgomery. But the prevailing thought is that it is an immune disorder.
New research suggests that psoriasis is a systemic disease that can affect any part of the body in which inflammation can spread, Wolfe said.
"Triggers of psoriasis include injuries, infection, stress, smoking, heavy alcohol use and certain blood pressure medicines," Wolfe said. "A family history of psoriasis is also a common theme."
Psoriasis increases risk for serious health conditions like diabetes, obesity, high blood pressure, cardiovascular disease and autoimmune diseases. It also can lead to depression.
Psoriasis comes in various forms, including plaque psoriasis – which has telltale thick, silvery scales – and erythrodermic psoriasis, in which most of the body reddens and becomes itchy and painful.
Plaque psoriasis normally develops on the elbows, knees or scalp, but it can appear on any part of the body. It tends to wax and wane at different times. Some people only will develop lesions on just a few skin surfaces while others will have the lesions across their bodies.
Erythrodermic psoriasis is the least common form, but it can result in a medical emergency especially for people with cardiac disease. This severe form of psoriasis can cause swelling from fluid retention and infection, increasing the risk of pneumonia and congestive heart failure.
It can also cause skin on most areas of the body to turn bright red and become itchy and painful. The skin sometimes falls off in sheets. People with unstable plaque psoriasis are most at-risk for developing it.
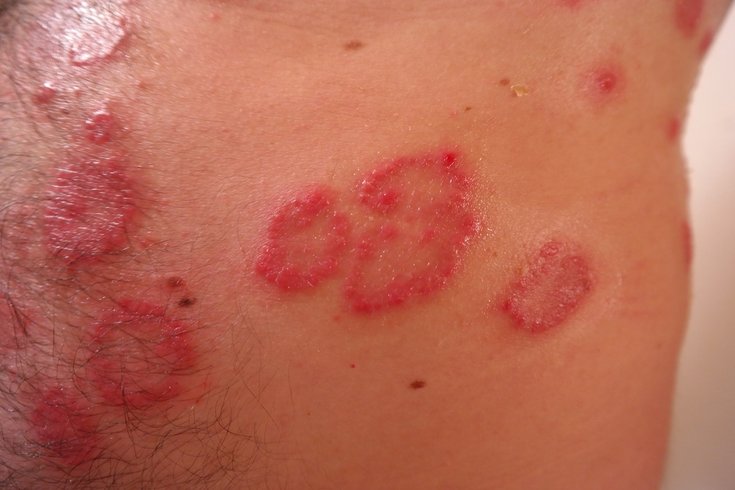
Other forms include nail psoriasis, which is identifiable by pitting in the nails or abnormal nail discoloration, and guttate psoriasis, which is similar to plaque psoriasis but results in more coin-shaped lesions. The latter form usually appears on the trunk of the body and is triggered by strep or another bacterial infection.
Inverse psoriasis, which occurs in the groin area and underneath the breasts and armpits, often is mistaken for a fungi infection. That can delay a patient from receiving the correct treatment.
Pustular psoriasis develops as white pustules of noninfectious pus that are surrounded by red skin, causing people to feel sick with fever and chills.
Additionally, some patients with psoriasis will develop lesions on areas that are not normally affected by the condition – a development known as the Koebner phenomenon.
Treatment options range from topical medications like corticosteroids, retinoids and vitamin D analogues to oral and injectable medications.
For more severe cases, narrow ultraviolet B phototherapy and photochemotherapy are used. Photochemotherapy requires patients to take light-sensitizing medicine before being exposed to UVB rays.
There also are biologic drugs made from living cells that target specific parts of the immune system, leading to better control of symptoms and better quality of life. They have changed the way psoriasis has been treated in the last 25 years, Wolfe said.
Anyone who develop psoriasis should talk to their doctor as soon as possible. Wolfe said, "If left untreated, psoriasis can make routine things uncomfortable and cause serious complications."